What happens to the body of a person who suffers from the long-term effects of the novel coronavirus?
A 33-year-old reporter for Kyodo News, my ailments related to COVID-19 continue to this day, more than a year after I recovered from the initial viral infection. Although I have seen slight improvements through treatment, I am still far from my former self.
Related coverage:
FEATURE: Japanese reporter describes agonizing long-term effects of COVID-19
In January, after an examination at the National Center of Neurology and Psychiatry in Tokyo, I was told I might be suffering from an immune disorder and reduced brain function due to the virus.
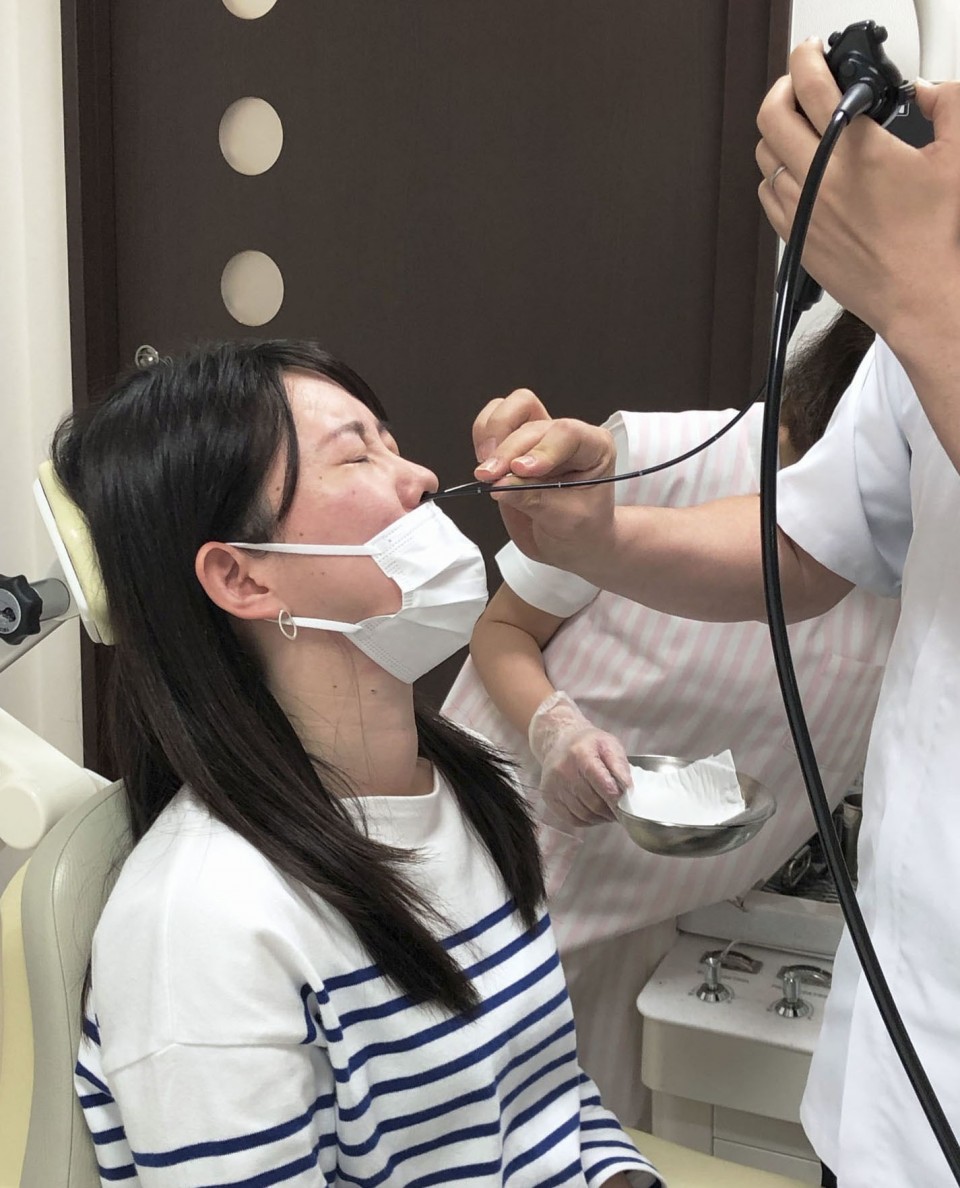
The exam I underwent included a brain perfusion scan, a test to determine blood flow in certain regions of the brain. It involves injecting radiotracers -- radioactive substances that emit tiny particles -- into a vein. A special camera is then used to track how the radioactive substance spreads throughout the brain to determine which areas are most active, which is believed to be indicated by blood supply.

The test can sometimes distinguish abnormalities in brain blood flow that a conventional MRI cannot detect and is also used in examinations for dementia.
My test results showed lower blood flow in the frontal and temporal lobes, which govern language and memory, than people in my age range.
According to Wakiro Sato, the head doctor in the center's immunology department who conducted the exam, brain function is thought to decline in areas of low blood flow. This tendency of reduced brain function is similar to the one found in many patients who have COVID-19 aftereffects.
No abnormalities were found when I underwent a brain checkup last August. And although I had suspected there might be a problem somewhere, I was left speechless in January by this worse-than-predicted outcome.
Why the drop in blood flow? "It is possible immune abnormalities occurred as a result of the infection, and blood flow deteriorated in connection with this," Sato told me.
After virus infections, "autoantibodies" that attack the body may form if the immune response does not subside, and this has already been confirmed in COVID patients with long-term aftereffects.
The center has long studied chronic fatigue syndrome, which causes various symptoms such as extreme fatigue and body aches. The presence of autoantibodies that disrupt the function of autonomic nerves is presumed to be one of the factors involved in chronic fatigue syndrome.
Sato said the center is applying the same knowledge to patients with long COVID, who exhibit many symptoms in common with CFS sufferers.
"Although they are few, some people with influenza do not fully recover. However, with COVID, there are many who don't, and this is why it is a particularly scary illness," Sato said.
There is no established cure for COVID-19. I have taken small amounts of prescribed steroids, among other treatments -- but it's a wait-and-see approach.
After articles about my experiences with the long-term effects of COVID-19 appeared in Japanese newspapers, people suffering from similar symptoms of long COVID posted their thoughts in messages on social media.
I was moved to tears to see that each person is fighting a lonely battle against an unknown illness. I plan to continue to speak out about the long-term effects of COVID-19 as I continue to receive treatment.
Related coverage:
Japan considering easing nonresident foreigner entry ban in March
Japan's COVID-19 death toll tops 20,000 amid Omicron spread
Japan approves Pfizer oral COVID-19 pill

 By Sayako Akita,
By Sayako Akita,









